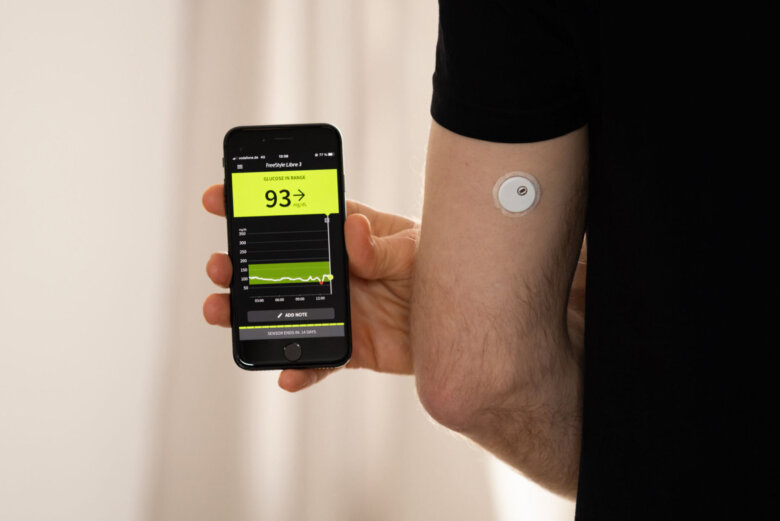
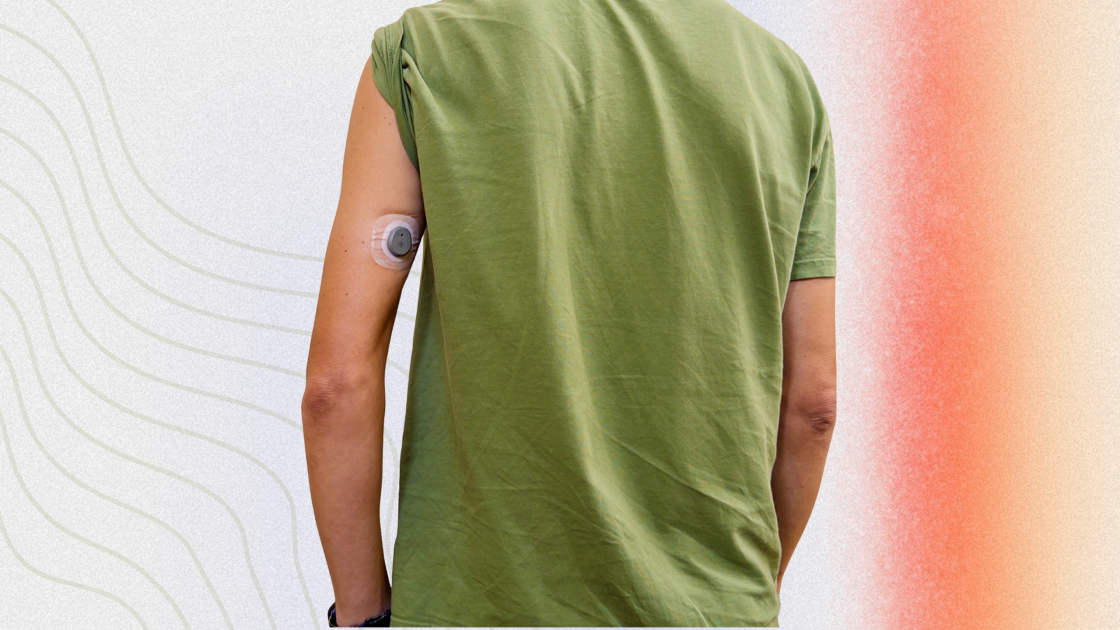
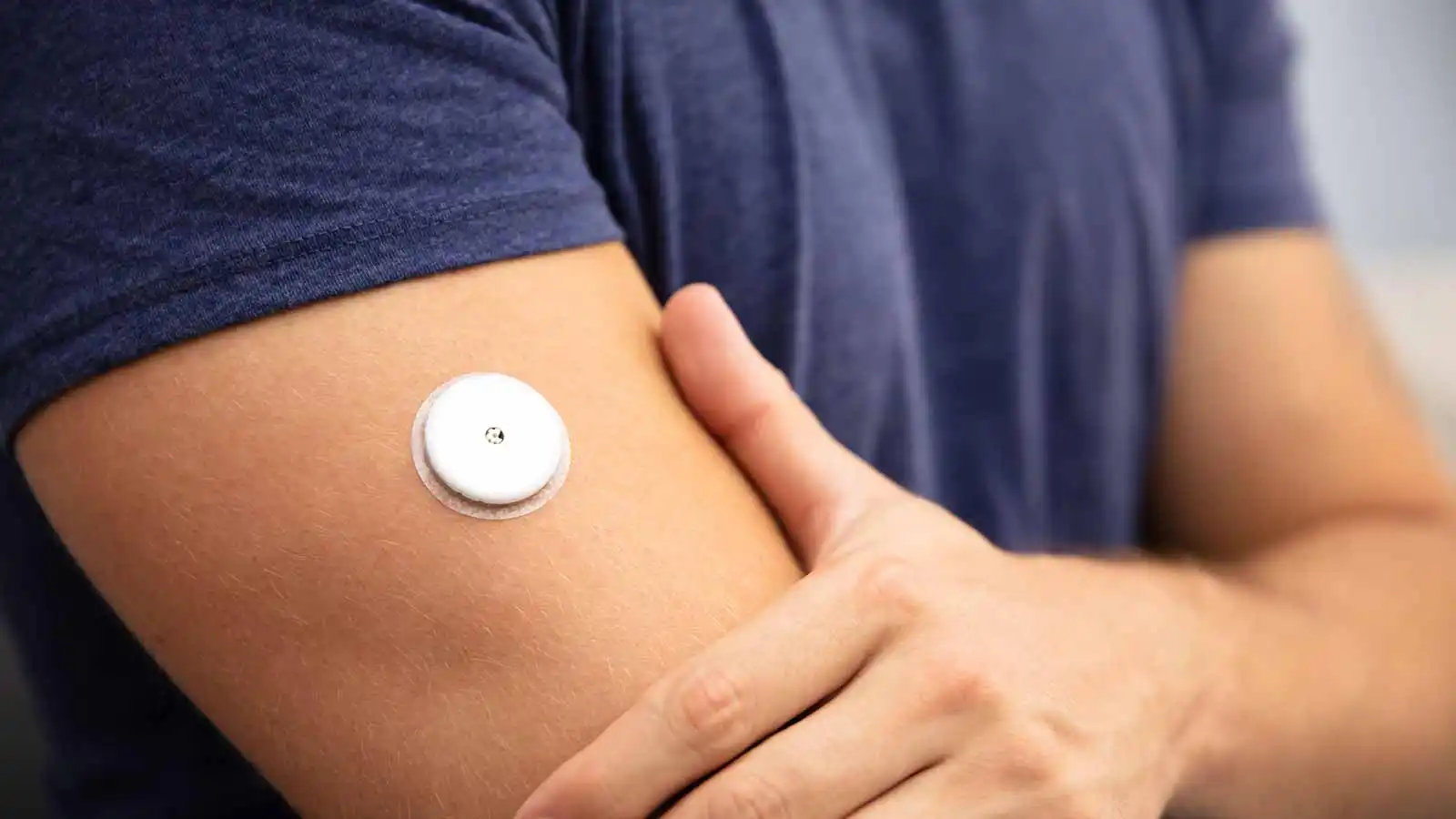
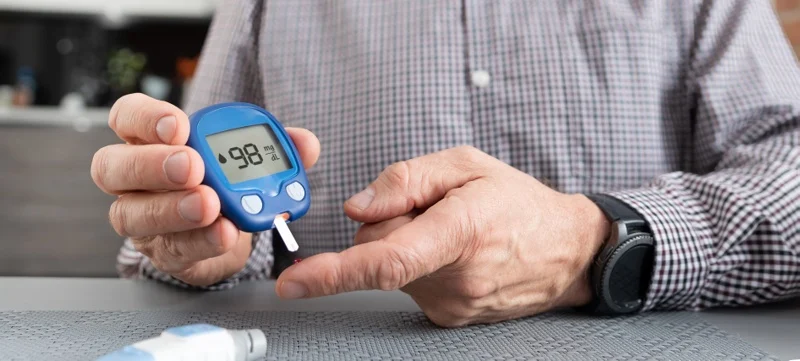
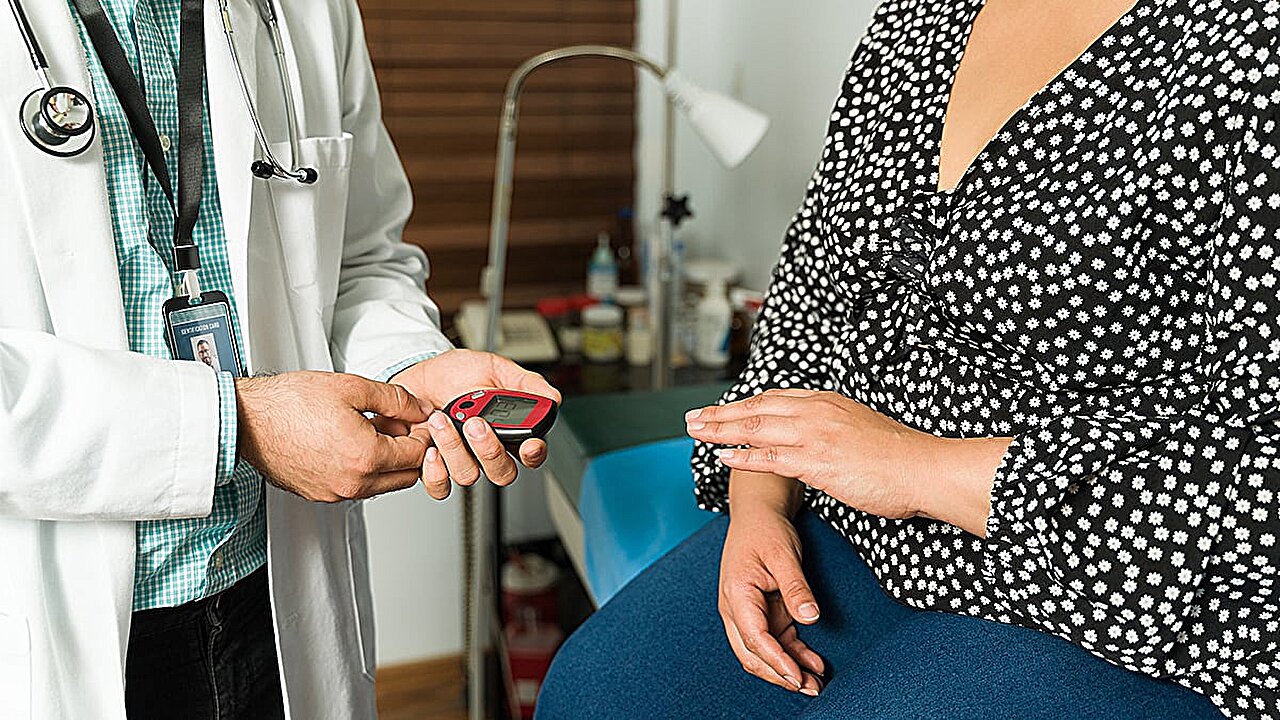
Continuous glucose monitors are wearable devices that track your blood glucose levels 24 hours a day and provide real-time data on trends. CGMs use a sensor inserted into the skin and a transmitter to provide glucose readings without the user moving — or pricking — a finger.
In the last 20 years, CGMs have become a lifesaving tool for people living with diabetes, which impacts how the body regulates blood sugar. The monitors can continuously and painlessly measure blood glucose and alert to spikes, so diabetics can take action and adjust insulin dosage.
However, CGMs have become increasingly popular among people who don’t have diabetes. Celebrities and influencers have touted CGMs for weight loss, energy and even athletic performance.
The devices are evolving into yet another trendy wearable gadget which promises to improve our health with more data. If we track our heart rate and steps, why not track blood sugar, too? Now, it’s easier than ever, because CGMs are no longer limited to people with diabetes.
In the last year, the U.S. Food and Drug Administration has approved multiple continuous glucose monitors for over-the-counter use, which means anyone can purchase them without a prescription, NBC News reported.
In August, the FDA approved the first over-the-counter glucose monitoring system for weight management. The system, from startup Signos, uses a monitor (the Dexcom Stelo) to measure glucose, along with an AI-powered platform to provide insights and personalized recommendations for behavior modifications.
Wearable hype and wellness influencers aside, do continuous glucose monitors actually help with weight loss or offer benefits for people without diabetes? We spoke to experts about how CGMs work and the potential risks and benefits.
What Are Continuous Glucose Monitors?
Continuous glucose monitors are small wearable devices that provide 24-hour monitoring of blood sugar levels.
Glucose is our body’s primary energy source and comes from the food we eat. Blood sugar refers to level of glucose in the bloodstream, which is regulated by the hormone insulin.
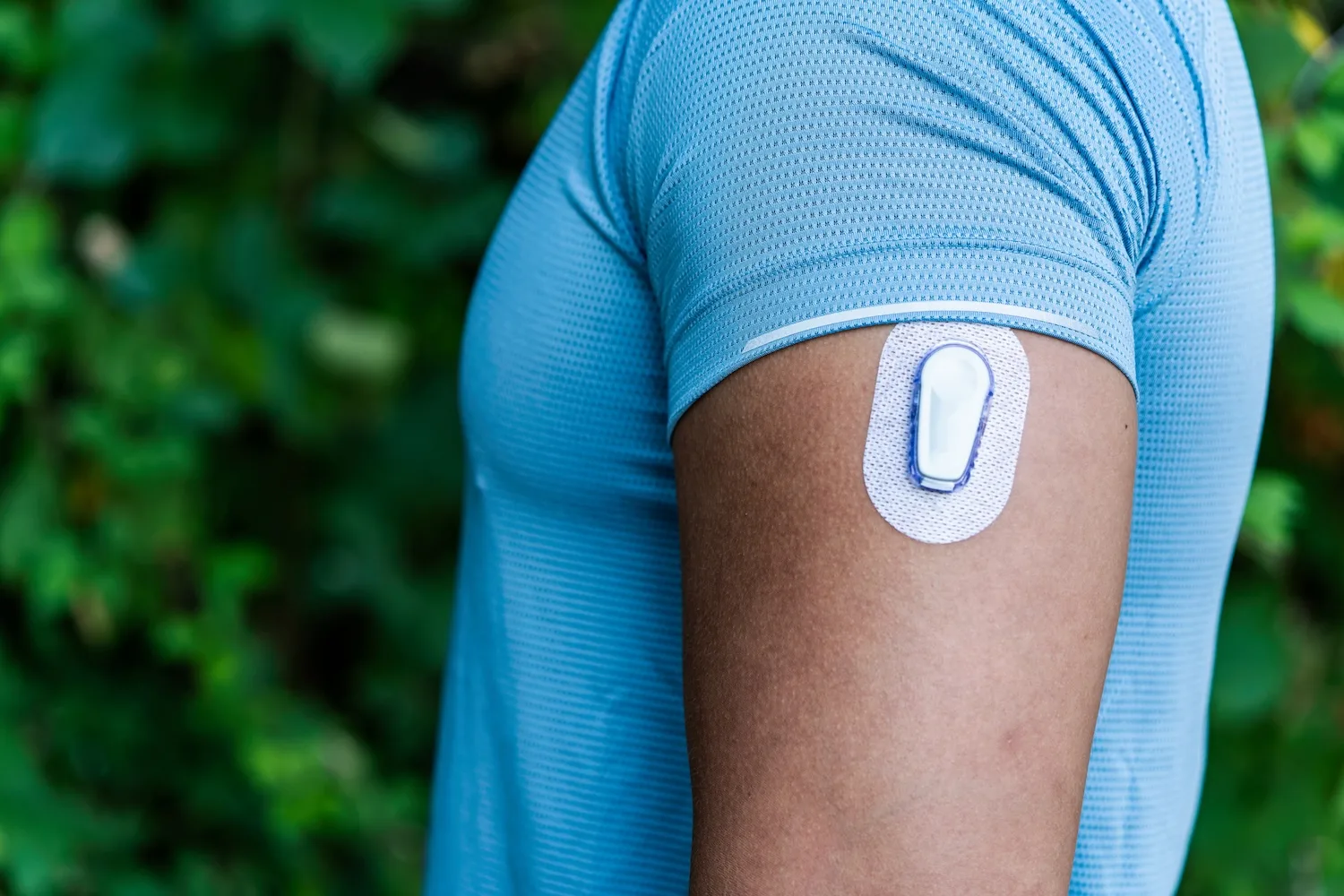
CGMs look like a quarter-sized patch which sticks to the skin, often placed on the upper arms or abdomen.
During application, a small needle inserts and retracts, leaving a tiny, flexible sensor in the skin, Dr. David Klonoff, endocrinologist and director of the Diabetes Research Institute at the Mills-Peninsula Medical Center (Sutter Health), tells TODAY.com.
The sensor records glucose concentrations about every 5 minutes, says Klonoff. It then transmits a wireless signal to a smartphone or wearable device, which gives you a glucose reading. CGMs are replaced every seven to 10 days.
How Do Continuous Glucose Monitors Work?
Instead of measuring glucose in the blood like traditional finger prick tests, CGMs measure the level inside the skin, in a fluid around cells called interstitial fluid, says Klonoff.
The concentration of glucose in interstitial fluid is very similar to the level in blood — but because glucose diffuses into the fluid from the bloodstream, there’s a slight lag in the CGM reading, Nicole Spartano, an assistant professor at Boston University School of Medicine, tells TODAY.com.
When blood sugar changes rapidly, it can take a few minutes for the CGM to pick up. “But it’s still representative of what is happening in the blood,” Spartano adds.
Whereas blood tests give a snapshot of glucose levels, CGMs can also track patterns, “so you can see your glucose levels rising or falling,” says Klonoff. This can show how blood glucose responds over time to factors like meals and physical activity.
CGMs are a powerful technology for people with diabetes, whose bodies cannot produce enough insulin or use it effectively, which leads to high blood sugar levels. They can help these individuals take preventive measures to prevent life-threatening spikes, per the American Diabetes Association.
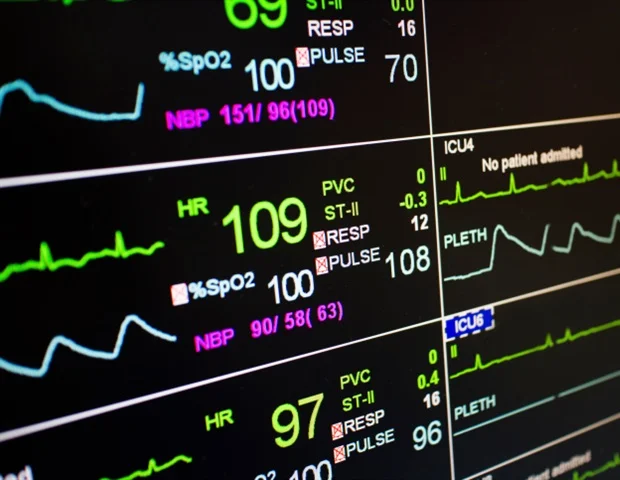
A “normal” blood glucose level for a healthy person is between 70 to 99 mg/dL, per the Cleveland Clinic.
People who do not have diabetes can use CGMs as an educational tool to measure their blood glucose and identify trends.
Now, companies like Signos are offering this technology with artificial intelligence that goes a step further by interpreting the CGM data for users and suggesting personalized behavior changes geared towards weight management.
“By revealing how food, exercise, sleep, stress, and more affect your body, it empowers users to build healthier habits,” Sharam Fouladgar-Mercer, Signos’ co-founder and CEO, tells TODAY.com via email. (Signos is not for the treatment of diabetes and not intended for use by people on insulin.)
Can CGMs Help With Weight Loss?
Continuous glucose monitors do not directly cause weight loss, the experts note. “There’s many steps that have to happen for it to actually lead to potential weight loss,” Collin Popp, P.hD., dietitian and assistant professor at the NYU Grossman School of Medicine, tells TODAY.com.
Theoretically, the insights from wearing a CGM could influence lifestyle choices, like diet and exercise, in a way that impacts a person’s weight. “It could help in a sense that it’s giving you feedback, and you can self-regulate,” says Popp.
However, this is highly dependent on the individual.
When approving the Signos system for weight management, the FDA also noted that it may “help the user better understand how lifestyle and behavior modification, including diet and exercise, impact glucose excursions. This information may be useful in helping users to maintain a healthy weight.”
The FDA added in a statement to TODAY.com: “While the (Signos) device may be useful in helping users to maintain a healthy weight, it was not cleared with a weight loss indication.”
Research on the effectiveness of CGMs for weight loss among people without diabetes is mixed and overall lacking.
In a 2022 study in JAMA Network Open co-authored by Popp, researchers compared outcomes among people on a personalized CGM-based diet versus a standard low-fat diet. “We found that it didn’t matter,” says Popp, adding that there was no significant difference in weight loss between both groups.
Fouladgar-Mercer points to a survey of 40 CGM users published in Clinical Diabetes in 2020, which showed that 90% felt that it contributed to a healthier lifestyle and 87% felt they changed their food choices based on CGM use. However, the study (which received funding from Dexcom) looked at subjects with diabetes.
When it comes to using CGM for weight loss or management in non-diabetic individuals, more studies are needed. “We might not be quite there yet in terms of the research,” says Spartano.
Of course, there are other ways to get personalized guidance to support weight loss — like seeing a health professional.
Do CGMs Have Benefits for Non-Diabetics?
The value of continuous glucose monitoring for people with diabetes is well-established. However, there isn’t enough scientific evidence to widely recommend the devices for healthy people who don’t have diabetes, the experts note.
“They are the final frontier, and we’re just not sure yet. We don’t have enough information,” says Klonoff.
Some non-diabetic people may find the devices help them make healthier lifestyle choices. But anecdotal evidence aside, there isn’t enough data to back up many of the trending claims about metabolism, energy or performance, the experts note.
“I’m not convinced that there is a real value for the general population,” Spartano adds.
However, research on the potential uses of CGMs is ongoing.
“There’s a potential promise in the diagnostic space and for risk prediction. … The devices might provide insight into flaws in your metabolic regulation,” Spartano adds.
CGMs may be helpful for people with prediabetes, which occurs when blood sugar is elevated but not high enough to be diagnosed as Type 2 diabetes. “There’s interest in the idea that you can prevent the progression to diabetes,” says Klonoff.
Although little data has been reported on the benefits of CGMs for people without diabetes, more well-designed clinical trials could help determine how these could play a role in the health of non-diabetics, according to a 2022 review in the Journal of Diabetes Science and Technology.
Risks of Continuous Glucose Monitors
Continuous glucose monitors are generally safe when used as directed by a doctor or as intended by a manufacturer, but there are potential downsides, the experts note.
The main risk of CGMs for non-diabetics is that the information can be overwhelming or cause anxiety. “There are people who can get so obsessed with the numbers, they lose sight of other things,” says Klonoff.
In some people, this could exacerbate disordered eating, Spartano warns.
Another potential issue is people misinterpreting or worrying over normal fluctuations in blood sugar. “People may think they shouldn’t have a glucose spike at all after they eat a meal. You should,” says Popp, adding that this could lead people to avoid healthy foods, such as fruit.
There’s also a small risk of inaccurate readings which could over- or underestimate blood glucose. “These devices are accurate, but they are not perfectly accurate,” says Klonoff.
While the device is generally painless, the adhesive can cause skin irritation or allergic reactions for some people, says Spartano. Rarely, the sensor can break off in the skin or cause an infection.
Finally, CGMs can be costly, especially if insurance doesn’t cover them. Depending on the brand, they may cost you thousands each year.
If you’re interested in using a CGM, talk to your doctor.